Private Healthcare Systems Network
- Just How your ConnectiCare® System American – PPO Plan Works
YOU SELECT COMPLETE SUPPLIER AND LEVEL OF ADVANTAGES
Your ConnectiCare system American PPO Plan enables you to pick the providers (health practitioners, hospitals, labs, etc.) for the health care services. Each time you require solutions, you might choose between providers just who take part in the Private medical care techniques, Inc. (PHCS) system (for in-network benefits) and the ones that do not take part in the community (for out-of-network advantages).
In-Network: If you use participating providers through the PHCS system, you are qualified to receive an increased, in-network standard of benefits. You will be responsible for a copayment at the time of solution. For most updated variety of participating providers, check out Find a health care provider, ConnectiCare’s on the web provider directory site or telephone call toll free: search by provider name, distance alongside traits which are more specific. (Participating providers for
Out-of-Network: If you use nonparticipating providers, you may well be qualified to receive a diminished out-of-network standard of advantages. You're going to be in charge of an annual deductible and coinsurance. Bear in mind, you’ll take full advantage of your benefits through the use of participating providers from the PHCS network.
COMPLETE PHARMACY ADVANTAGES when your program features a prescription medicine driver, you are eligible for prescription medication benefits. When using a participating drugstore or our mail-order drugstore seller, you will be accountable just for the applicable copayment. When making use of a nonparticipating drugstore, you're going to be in charge of having to pay the entire price of your prescription at drugstore. We're going to reimburse you for covered prescription medications at our optimum Allowable Amount.**
FILING CLAIMS When you receive solutions from a participating supplier or drugstore, there is no need is worried about processing a claim. A participating supplier or pharmacy will collect your copayment from you during service and file the claim in your stead.
Once you obtain services from a nonparticipating provider/pharmacy, you must send us a completed claim form (forms can be obtained online at or from your own group advantages administrator), along with reveal bill from your supplier or drugstore. We will process the claim and, in case it is payable, reimburse you based on the proper benefit amount. (If the provider or pharmacy presented the claim on your behalf, we are going to issue repayment towards supplier.)
We ought to obtain claims within 180 times from the time the solution, medication or offer was obtained. Claims received over 180 times following the time will never be reimbursed.
Share this Post
Related posts
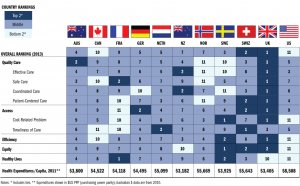
Best Healthcare Systems in the World
Luxembourg City in the winter.Barbara TaschThe Legatum Institute, a London-based study institute released its 10th yearly…
Read MoreGonzales Healthcare Systems
Gonzales Healthcare Systems in Gonzales, Texas plays an important role in the distribution of healthcare services towards…
Read More